[ad_1]
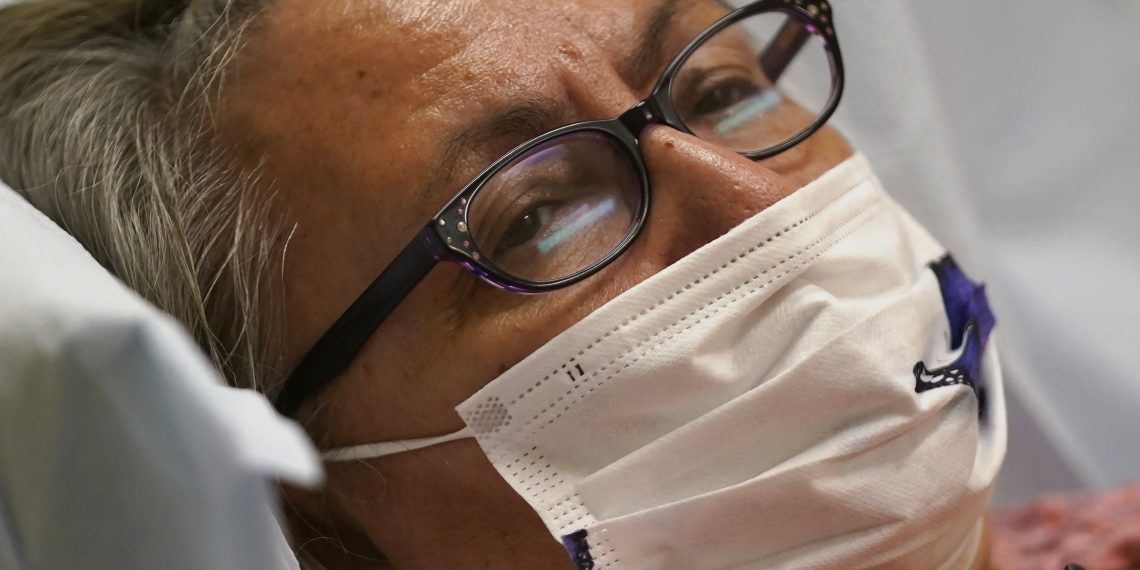
Joyce Johnson-Albert appears to be like on as she receives an antibody infusion whereas mendacity on a mattress in a trauma room on the Higher Tanana Well being Middle Wednesday, Sept. 22, 2021, in Tok, Alaska.
Rick Bowmer | AP
Dr. Jeremy Gitomer at Windfall Alaska Medical Middle in Anchorage realized final month there weren’t sufficient dialysis machines to deal with the flood of Covid sufferers affected by renal injury.
One intubated 70-year-old lady, who was additionally battling kidney failure and was on dialysis for six days, wasn’t prone to make it, he recalled.
Gitomer and his medical staff determined to terminate her therapy to release the machine for a 48-year-old man who was additionally on a ventilator and had a better likelihood of restoration if given dialysis. Each sufferers died ultimately, he stated, including that as much as 95% of intubated Covid sufferers on dialysis don’t survive in Alaska.
“It is horrible that I am dwelling via this as a result of I’ve by no means seen extra individuals die in my profession,” stated Gitomer, a nephrologist who works at Anchorage’s three hospitals for the Kidney and Hypertension Clinic of Alaska. “I have been doing this 25 years.”
Docs at Windfall have been compelled to decide on who may dwell and who will seemingly die as a crush of Covid sufferers stretches the hospital’s restricted assets to capability.
Angie Cleary, a registered nurse, cares for Joyce Johnson-Albert as she receives an antibody infusion whereas mendacity on a mattress in a trauma room on the Higher Tanana Well being Middle Wednesday, Sept. 22, 2021, in Tok, Alaska.
Rick Bowmer | AP
Alaska is within the thick of a surge of instances fueled by the extremely contagious delta variant, which devastated the continental U.S. over the summer time. To alleviate the burden on the state’s health-care system, Alaskan officers on Oct. 2 activated “disaster requirements of care” throughout 20 hospitals, a measure that provides them some authorized safety if they’ve to decide on who will get a mattress or ventilator which will save a affected person’s life whereas they forgo therapy for others who’re much less prone to survive.
Anchorage hospitals, the place practically all the state’s dialysis machines are situated, have been compelled to reject transfers of sufferers who’ve a low likelihood of survival from different in-state medical facilities, Gitomer stated. It is not simply placing Covid sufferers at increased danger. Hospitals at the moment are struggling to deal with non-Covid sufferers with a variety of life-threatening situations, together with most cancers, accident accidents and organ failure. Sufferers with mind tumors face prolonged emergency room delays, prolonging their means to get an MRI and see a neurosurgeon, docs say.
Mat-Su Regional Medical Middle, situated some 40 miles northeast of Anchorage, cannot simply switch renal and coronary heart failure sufferers to Anchorage prefer it often does. The hospital now has to maintain a few of them in a single day and “effectively sufficient to make it for outpatient dialysis the following day,” stated Dr. Anne Zink, the state’s chief medical officer and an emergency room doctor at Mat-Su.
“As an alternative of 1 nurse with the ability to look after 4 or 5 emergency division sufferers, they could be caring for 10 emergency division sufferers,” Zink stated of Mat-Su, the place Covid sufferers occupy nearly half of the hospital’s 100 beds. “Sufferers having to board within the emergency division anticipate a very prolonged time period.”
Alaska, which has managed dozens of Covid instances at any time all through many of the outbreak, had greater than 1,200 new instances Wednesday — peaking at a seven-day common of 1,317 new instances on Sept. 27, in accordance with a CNBC evaluation of knowledge from Johns Hopkins College. Alaska is the third-least populous state within the nation, but it surely at present has essentially the most Covid instances per particular person at 120 new infections per 100,000 residents as of Wednesday. And Covid sufferers are crowding hospital beds at nearly twice the speed of the nationwide common, in accordance with information from the Division of Well being and Human Companies.
Alaska’s sheer geographic vastness additional complicates the state’s means to battle the outbreak: Well being-care facilities are so unfold out that the common Alaskan should journey about 150 miles a technique for medical consideration, Zink stated. Mat-Su Regional Medical Middle alone companies an space the dimensions of West Virginia.
The state introduced in 400 out-of-state medical personnel late final month to assist with the surge, Zink stated.
A mix of faculty resuming, snow falling and other people spending extra time indoors has made Alaska notably weak to the extremely transmissible delta variant this fall, Zink stated. Many communities additionally lacked entry to working water and sewers and confronted excessive charges of respiratory ailments earlier than the pandemic even started, she defined, elevating their danger for a Covid outbreak.
“We’re seeing way more dying and dying with this surge,” stated Dr. Angelique Ramirez, chief medical officer at Basis Well being Companions in Fairbanks. “It is taking place every day, it is taking place in youthful individuals, and it is taking place regardless of the whole lot we all know tips on how to do.”
Vaccine hesitancy runs excessive in Alaska, making monoclonal antibodies a preferred Covid therapy, Ramirez stated. However as the provision of antibodies dwindled with the surge, Ramirez stated Basis Well being was compelled to order the lifesaving therapy for less than essentially the most weak sufferers.
Herbie Demit, Tanacross Village Council president, walks via a cemetery Thursday, Sept. 23, 2021, in Tanacross, Alaska. Alaska is experiencing one of many sharpest rises in COVID-19 instances within the nation, coupled with a restricted statewide healthcare system that’s nearly solely reliant on Anchorage hospitals.
Rick Bowmer | AP
“When it grew to become scarce, we had a option to make,” Ramirez stated. “And our selection was we might both dissipate all we had and easily run out, or we might select to take a look at who was utilizing it and make selections off of it at a neighborhood stage as to who would most profit from it and restrict it to these people.”
Staffing crunches at Basis Well being have lowered capability, Ramirez stated. The hospital has been suspending non-emergency surgical procedures and discharging pneumonia sufferers sooner than regular, equipping them with at-home oxygen remedies as soon as docs are comfy with their restoration quite than holding them till they’ve absolutely recuperated, she stated.
Ramirez blamed the surge in Fairbanks on the area’s low vaccination fee and public resistance to sporting masks. And regardless that Ramirez stated the surge started earlier than faculties began for the 12 months, she stated she anticipated the return to in-person studying would exacerbate the outbreak.
Alaska has vaccinated greater than 51% of its inhabitants towards Covid, rating thirty fifth within the nation amongst all states and Washington, D.C., as of Wednesday, in accordance with the CDC. Misinformation and anti-vaccine sentiment have confirmed important obstacles within the push to immunize extra Alaskans, stated Charlee Gribbon, a nurse and an infection preventionist at Bartlett Regional Hospital in Juneau.
“Viruses are a tough pathogen to regulate,” Gribbon stated. “So after we pull out all of the stops, we simply want all people to assist us out with no matter they’ll do to keep away from spreading the sickness.”
— CNBC’s Nate Rattner contributed to this report.
[ad_2]
Source link